Resources

FAQ: How to Teach a Procedural Skill
Why is it important to teach procedural skills in general practice?
Procedural skills are an essential part of general practice, particularly in rural and remote settings. Teaching these skills helps maintain a broader scope of care, supports registrar confidence, and ensures patient access to timely procedures.
What is the difference between teaching procedural and other skills?
The major difference between a procedural skill and a communication (or interview) skill is that it is assigned to “muscle memory” and does not require conscious thought except at key steps. Because of this, supervisors often have difficulty identifying how they learnt a procedural skill in order to teach it to others regardless of how expert they are at that particular procedure.
What are the three key stages of learning motor skills?
Fitz and Posner identified three key stages of learning motor skills:
- Cognitive – when movements are being learnt they are slow and clumsy due to being consciously controlled.
- Associative stage – some of the movements are automatic and fluid but others require executive oversight and are slow and jerky.
- Autonomous stage – Fluid, accurate and fast movements.
What is the first step in teaching a procedural skill?
The breakdown of a procedural skill can be achieved by task analysis in which the supervisor:
- Visualises the procedure
- Writes down the key steps
- Motor skills (what the hands do)
- Cognitive steps (what the mind must consider)
- Decision-making points (critical judgments or pitfalls)
- Reconstructs the task and see if anything is missing
This becomes the foundation for teaching, feedback, and assessment.
WHAT IS A COMPETENCY CHECK LIST?
A competency checklist lists all the key steps and can be used as an assessment tool. For example,
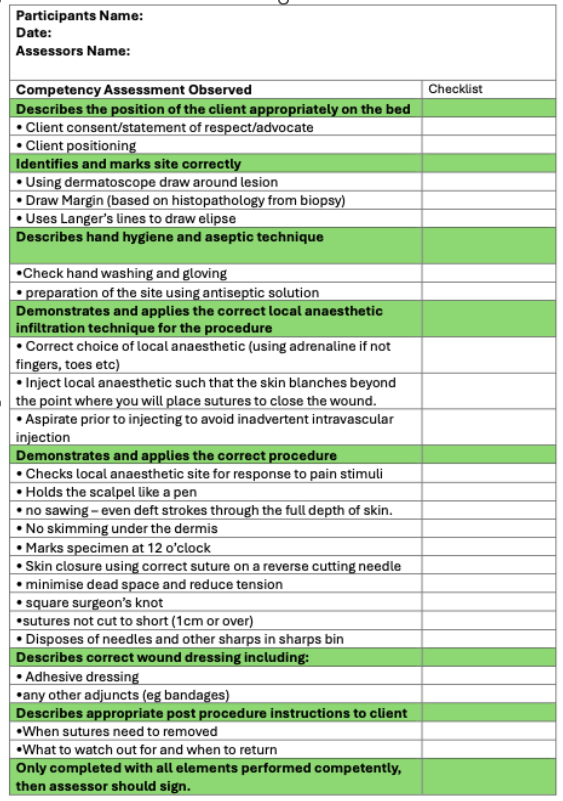
HOW DO I STRUCTURE PROCEDURAL SKILL TEACHING FOR REGISTRARS?
A modified Peytons method can then be applied to the teaching process which is a advance on the “see one, do one teach one” philosophy often used in medicine.
- Demonstration. This involves the facilitator demonstrating the skill in real time without any explanation or commentary.
- Deconstruction. The facilitator performs the procedure again, this time breaking in down into sub-steps and explaining each step.
- Comprehension. In this step, the facilitator asks the participant to explain the procedure to the facilitator and the facilitator performs the procedure following the participants instructions.
- Performance. In the final step, the participant performs the procedure on their own without coaching or guidance by the facilitator.
- Error correction – verbal guidance increases cognitive load but it is important that any errors identified in skills are corrected as they occur
- Incorporate visual aids, simulation, and checklists where appropriate.
HOW DO I MANAGE THE COGNITIVE LOAD FOR LEARNERS?
Break the skill into small, digestible components. Avoid overloading registrars with too much feedback at once. Focus on one or two key points per session and offer timely, concise feedback.
HOW DO I KNOW IF MY REGISTRAR IS READY TO PERFORM A PROCEDURE INDEPENDENTLY?
Use your task analysis to build a competency checklist. This allows you to:
- Objectively assess performance
- Identify knowledge gaps
- Ensure consistency in teaching and evaluation
Registrars should demonstrate conscious competence before unsupervised practice.
WHAT IS "DELIBERATE PRACTICE" AND WHY IS IT IMPORTANT?
Deliberate practice involves intentional, repetitive performance of a task with immediate feedback and supervision. It’s essential for:
- Consolidating skills into long-term memory
- Transitioning to unconscious competence
- Maintaining procedural confidence over time
Plan regular practice sessions, even after initial competence is achieved.
WHAT IF MY REGISTRAR LACKS CONFIDENCE OR REFUSES TO DO CERTAIN PROCEDURES?
Explore underlying reasons—cultural, emotional, or confidence-based. Create a safe learning environment, provide non-judgmental debriefing, and consider alternative approaches like:
- Simulation or models
- Peer discussion or yarning circles
- Reframing the procedure’s purpose or patient benefit
HOW DO I INCLUDE PATIENT-CENTRED CARE IN PROCEDURAL TRAINING?
Ensure registrars understand the importance of:
- Informed consent (explain risks/benefits, gain genuine agreement)
- Respectful communication (put the patient at ease)
- Post-procedure care (follow-up, aftercare instructions, recall systems)
These non-technical skills are as vital as the procedure itself.
HOW DO I TEACH IF I’VE LOST CONFIDENCE IN A SKILL MYSELF?
Refresh your skills using:
- Peer review or mentorship
- Simulation or workshops
- High-quality procedural videos (YouTube, vetted medical channels)
It’s okay to learn alongside your registrar—and it models good professional behaviour.
ARE ALL PROCEDURES SUITABLE FOR THIS APPROACH?
Yes. While often associated with surgical or invasive tasks, any procedural or physical skill—from PR exams to wound care or contraceptive insertion—can and should be taught using a structured, stepwise, patient-centred approach.
WHAT TOOLS OR RESOURCES CAN I USE TO SUPPORT THIS?
- Task analysis worksheets
- Checklists based on skill steps
- DOPS (Direct Observation of Procedural Skills) forms
- Simulation models
- Visual aids and diagrams
- Trusted online video tutorials
WHAT IS A FINAL TIP FOR SUPERVISORS?
Remember: You are unconsciously competent. To teach well, slow down, unpack each step, and build the procedure from the ground up. Be the bridge from “not yet” to “I’ve got this.”
REFERENCES
- Benner, P. (1982). From Novice to Expert. The American Journal of Nursing, 82(3), 402–407.
- Bing-You, R., Hayes, V., Varaklis, K., Trowbridge, R.,
- Kemp, H., & McKelvy, D. (2017). Feedback for Learners in Medical Education: What Is Known? A Scoping Review. Academic Medicine, 92(9), 1346–1354.
- Bosse, H. M., Mohr, J., Buss, B., Krautter, M., Weyrich, P., Herzog, W., Jünger, J., & Nikendei, C. (2015). The benefit of repetitive skills training and frequency of expert feedback in the early acquisition of procedural skills. BMC Medical Education, 15(1), 22–22.
- Burgess, A., van Diggele, C., Roberts, C., & Mellis, C. (2020). Tips for teaching procedural skills. BMC Medical Education, 20(Suppl 2), 458–458.
- Dreyfus, S. E., & Dreyfus, H. L. (1980). A five-stage model of the mental activities involved in directed skill acquisition. Distribution 22.
- Ericsson, K. (2008). Deliberate Practice and Acquisition of Expert Performance: A General Overview. Academic Emergency Medicine, 15(11), 988–994.
- Frank, J. R., Snell, L. S., Cate, O. T., Holmboe, E. S., Carraccio, C., Swing, S. R., Harris, P., Glasgow, N. J., Campbell, C., Dath, D., Harden, R. M., Iobst, W., Long, D. M., Mungroo, R., Richardson, D. L., Sherbino, J., Persky, A. M., & Robinson, J. D. (2017). Moving from Novice to Expertise and Its Implications for Instruction. American Journal of Pharmaceutical Education, 81(9), 6065–6080.
- Johnson, J., Ahluwalia, S. Neurodiversity in the healthcare profession, Postgraduate Medical Journal, Volume 101, Issue 1192, February 2025, Pages 167–171
Peyton JWR (1999). The learning cycle. In: Peyton JWR, editor. Teaching and learning in medical practice. Rickmansworth: Manticore Europe Ltd; p. 13–9. - Quinn, A., Falvo, L., Ford, T., Kennedy, S., Kaminsky, J., & Messman, A. (2021). Curated collections for educators: Six key papers on teaching procedural skills. AEM Education and Training, 5(4), e10692-n/a.
- Sawyer, T., White, M., Zaveri, P., Chang, T., Ades, A., French, H., Anderson, J., Auerbach, M., Johnston, L., & Kessler, D. (2015). Learn, See, Practice, Prove, Do, Maintain: An Evidence-Based Pedagogical Framework for Procedural Skill Training in Medicine. Academic Medicine, 90(8), 1025–1033.
- Schnotz, W. (2010). Reanalyzing the expertise reversal effect. Instructional Science, 38(3), 315–323.
Silver, I., Taber, S., Talbot, M., & Harris, K. A. (2010). Competency-based medical education: theory to practice. Medical Teacher, 32(8), 638–645. - Telio, S., Ajjawi, R., & Regehr, G. (2015). The “Educational Alliance” as a Framework for Reconceptualizing Feedback in Medical Education. Academic Medicine, 90(5), 609–614.
Tremblay, M., Rethans, J., & Dolmans, D. (2023). Task complexity and cognitive load in simulation‐based education: A randomised trial. Medical Education, 57(2), 161–169. - van Merrienboer, J. J. G., & Sweller, J. (2010). Cognitive load theory in health professional education: design principles and strategies. Medical Education, 44(1), 85–93.
- Weallans, J., Roberts, C., Hamilton, S., & Parker, S. (2022). Guidance for providing effective feedback in clinical supervision in postgraduate medical education: a systematic review. Postgraduate Medical Journal, 98(1156), 138–149.
- Wearne, S., Australian Family Physician (2011) Vol. 40, 63-67
Date reviewed: 02 February 2026
Please note that while reasonable care is taken to provide accurate information at the time of creation, we frequently update content and links as needed. If you identify any inconsistencies or broken links, please let us know by email.